About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。

If you can't understand the subsequent professional descriptions, just take two minutes to read through this text
Overview of the condition
knowledge
The most common pathological type of kidney cancer is renal clear cell carcinoma, which is composed mostly of clear cells, hence the name clear cell carcinoma.
Painless hematuria throughout the entire urination process is a characteristic of kidney cancer. Pain may also occur in kidney cancer, but it is mostly located in the kidney area, commonly referred to as the "lower back" by the general public. However, in recent years, most kidney cancer patients are found to have asymptomatic kidney cancer during health check-ups, accounting for more than 50% to 60% of all kidney cancer patients. Therefore, regular physical examinations are of great significance for early detection and treatment.

1. The patient was diagnosed with renal clear cell carcinoma and underwent radical surgery in a timely manner. Post-surgery chemotherapy for renal cancer exhibits significant individual variability, with most patients being insensitive to chemotherapy. Mr. Chen chose not to undergo chemotherapy.
2. However, renal cancer is sensitive to immunotherapy, such as NKT cell therapy, anti-PD-1 monoclonal antibody, and anti-PD-L1 monoclonal antibody. For patients who cannot undergo traditional chemotherapy after surgery, immunotherapy provides a new option. Mr. Chen chose dendritic cell vaccine post-surgery and maintained stability for four years, which sufficiently demonstrates this point.
3. However, subsequent metastatic lesions were found in the lungs and brain, indicating that immunotherapy needs to be continuous and cannot be taken lightly.
4. Radiotherapy treatment reduced the tumor burden to some extent, but the tumor progressed afterwards, requiring additional therapeutic intervention. NKT therapy has few side effects and can be administered after radiotherapy has reduced the tumor burden to delay tumor progression.
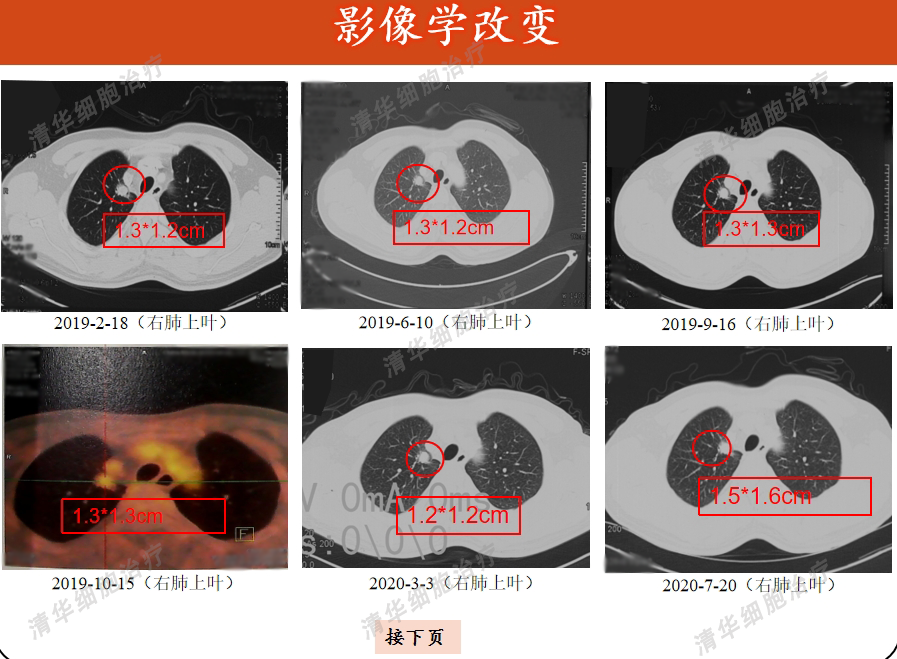
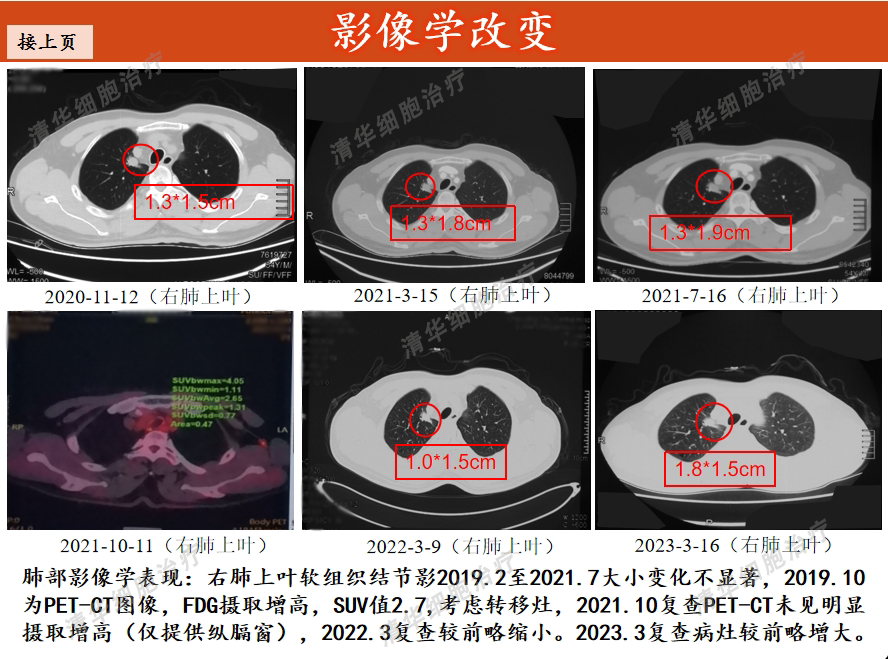
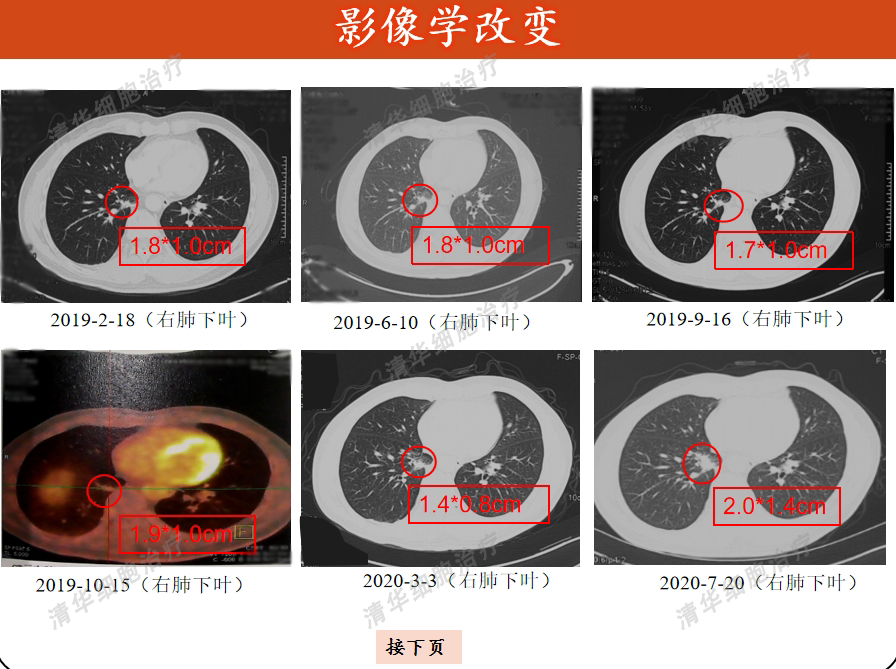
Image aspect
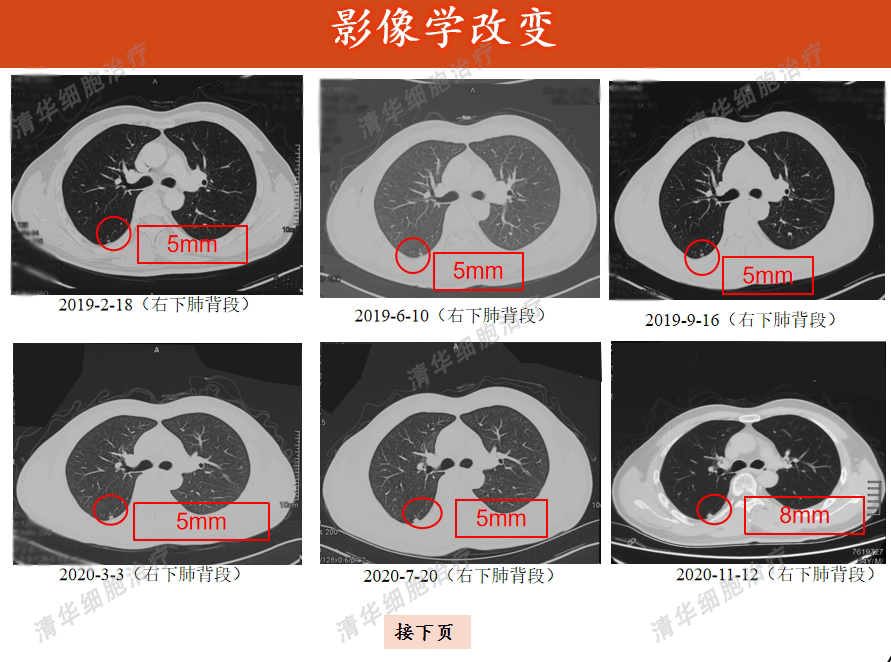
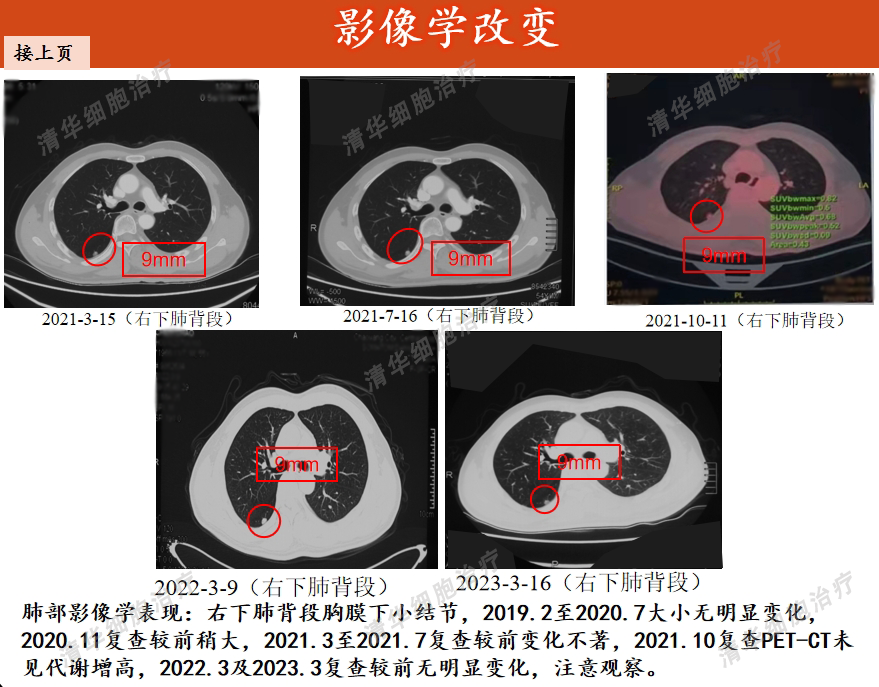
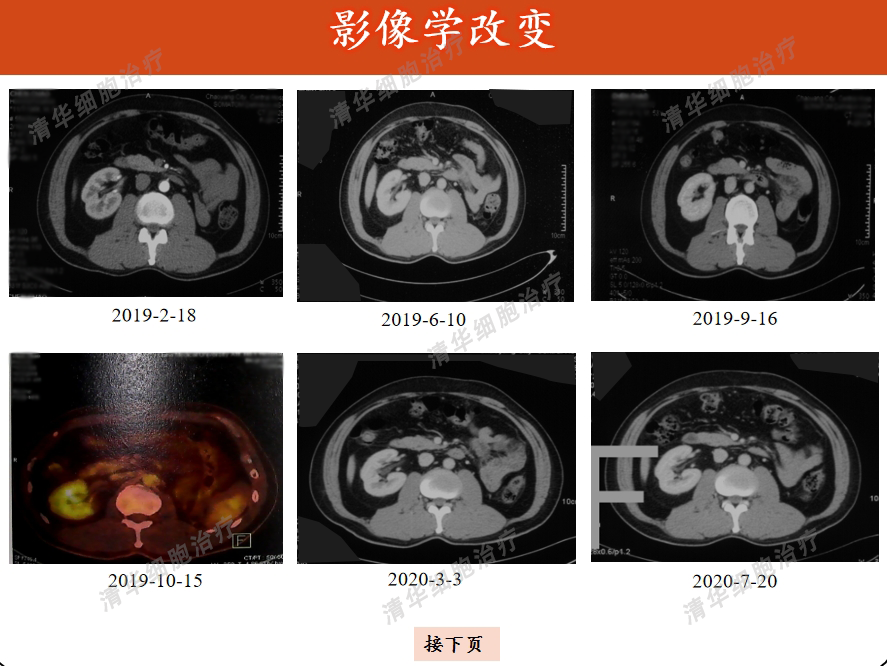
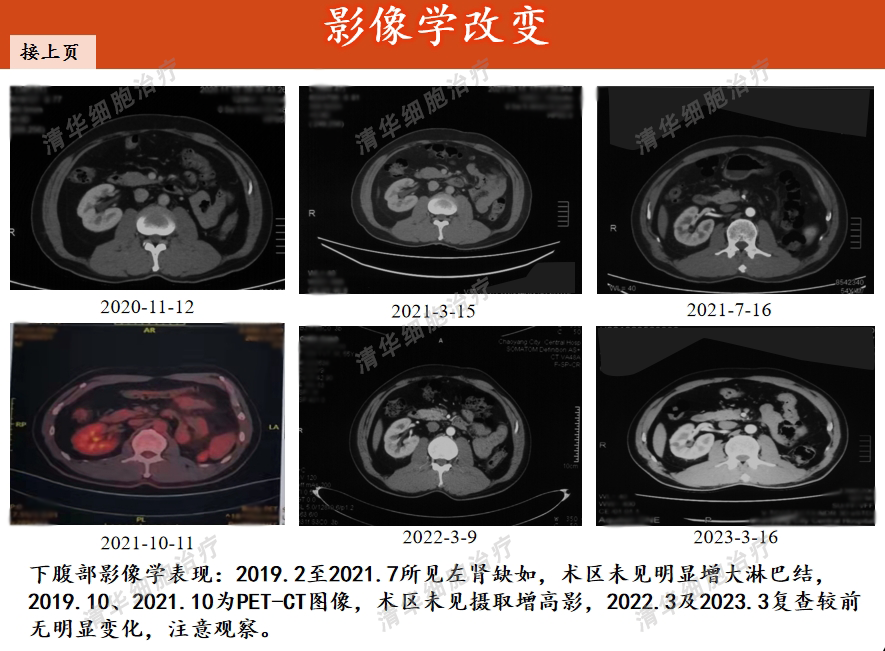

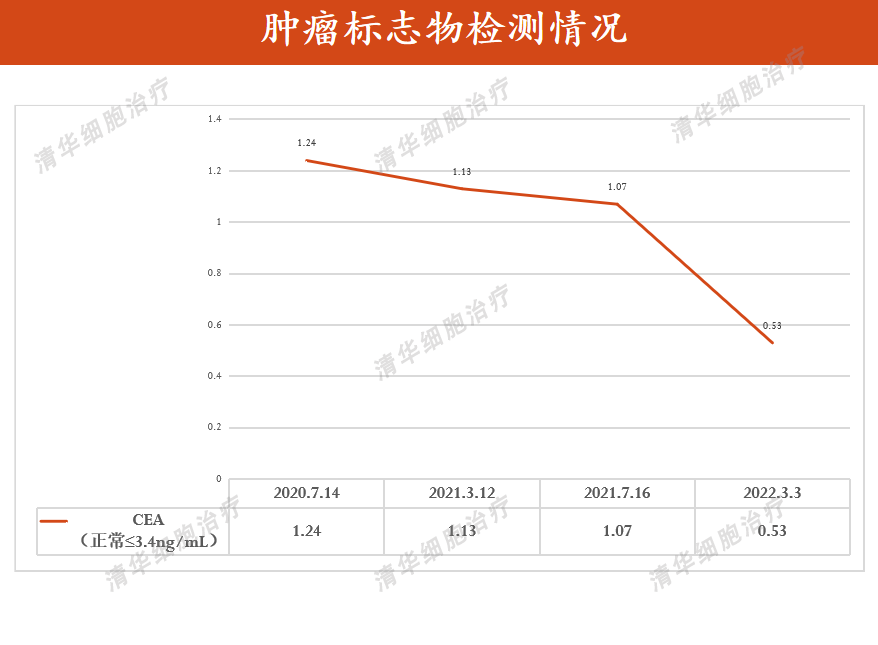
Tumor markers
Normal range of tumor marker CEA from July 2020 to March 2022.
Conclusion and Comments
Reference:< H383>
【1】Kidney cancer with brain metastases. Prognostic factors and treatment outcome.A V Golanov , S M Banov , E R Vetlova , O N Dreval , A K Bekyashev , S R Iliyalov , N A Antipina , A A Durgaryan , A A PogosovaVoprosy onkologii Pub Date : 2016-01-01
Click on the image