About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。
Cancer is not terrifying; it can be prevented and treated. The key lies in having the right mindset and scientific methods!
— Tsinghua University. Zhang Minghui
01
Case Analysis
If you cannot understand the subsequent professional description
you can finish reading this text in two minutes
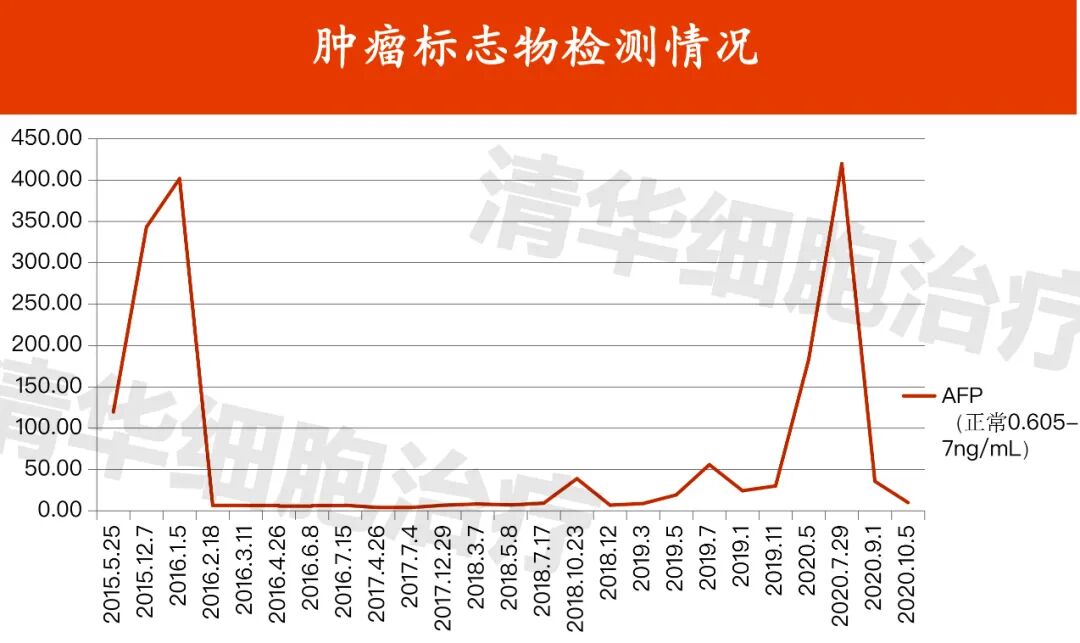
Brief Introduction to Mr. Lei's Condition
Mr. Lei is such a patient who often suffers from the counterattack of illness, but due to appropriate treatment strategies and timely intervention, he has successfully turned his dangerous liver cancer into a "chronic disease".
In September 2011, Mr. Lei was found to have intrahepatic space-occupying lesions and underwent tumor resection in October of the same year. The diagnosis was liver cancer with intrahepatic metastasis, and the postoperative pathology showed moderately differentiated hepatocellular carcinoma. He was also treated with antiviral therapy and traditional Chinese medicine.
About two and a half years later, intrahepatic recurrence was found. Starting from January 2014, he underwent six consecutive transcatheter arterial chemoembolization (TACE) procedures for control.
In March 2015, a new lesion was found in the left lateral lobe of the liver, and TACE was performed again for control. Two months later, another new liver cancer sub-lesion was found, and TACE was still used for treatment. After two months, a PET-CT scan was performed, and it was considered that the right lobe of the liver still had tumor activity. Therefore, in December 2015, he underwent cyberknife treatment.
The repeated recurrence of intrahepatic lesions four times has caused Mr. Lei great suffering, and the intervals between recurrences are very short. It can be seen that the cancer cells are very active and aggressive. If there is no effective treatment to suppress them, it is likely that his body will not be able to withstand the next recurrence.
02
Treatment Overview
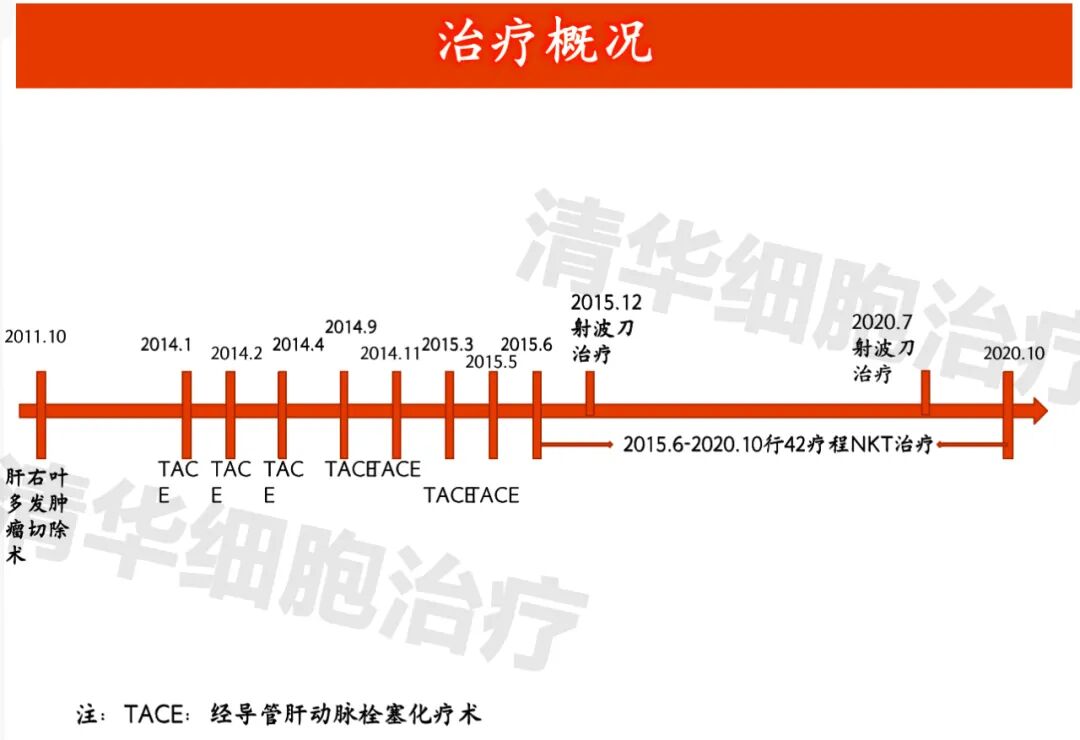
Treatment Overview of Mr. Lei
03
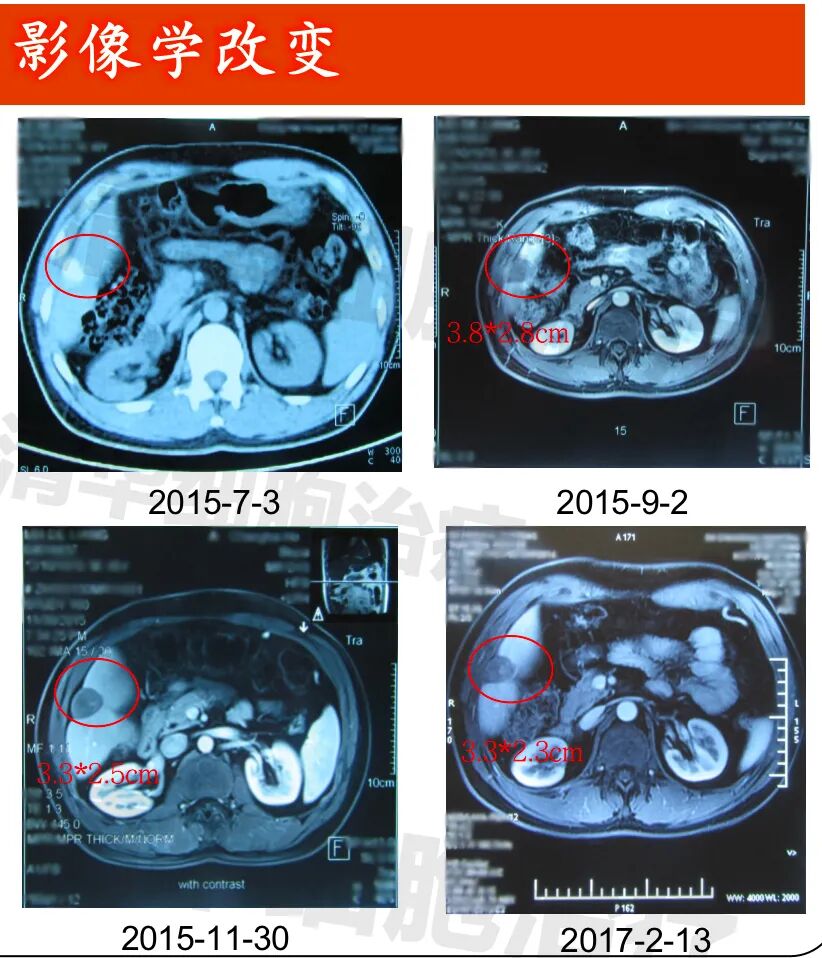
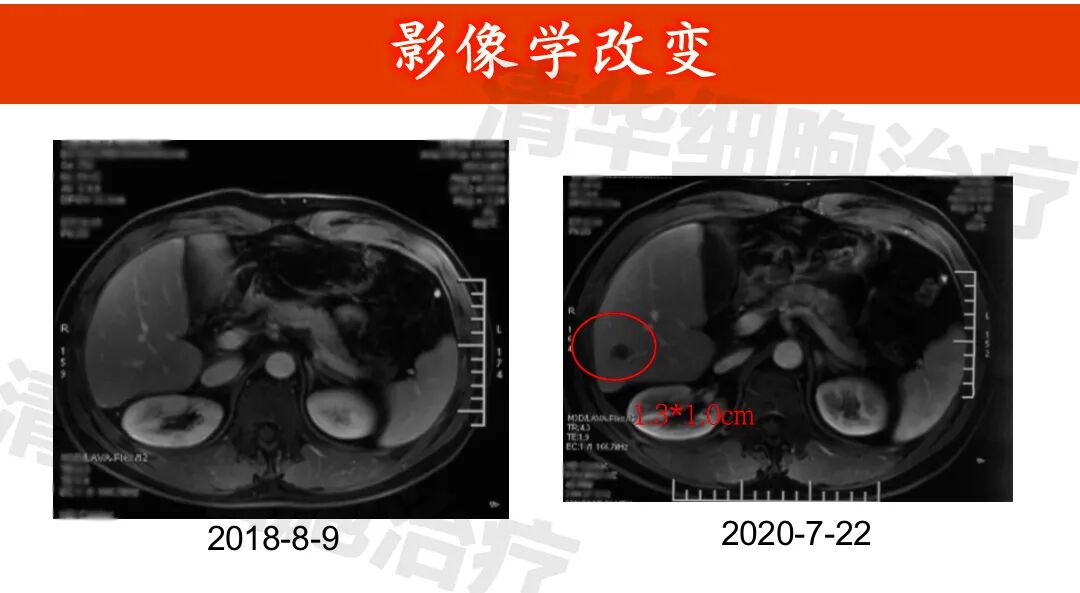
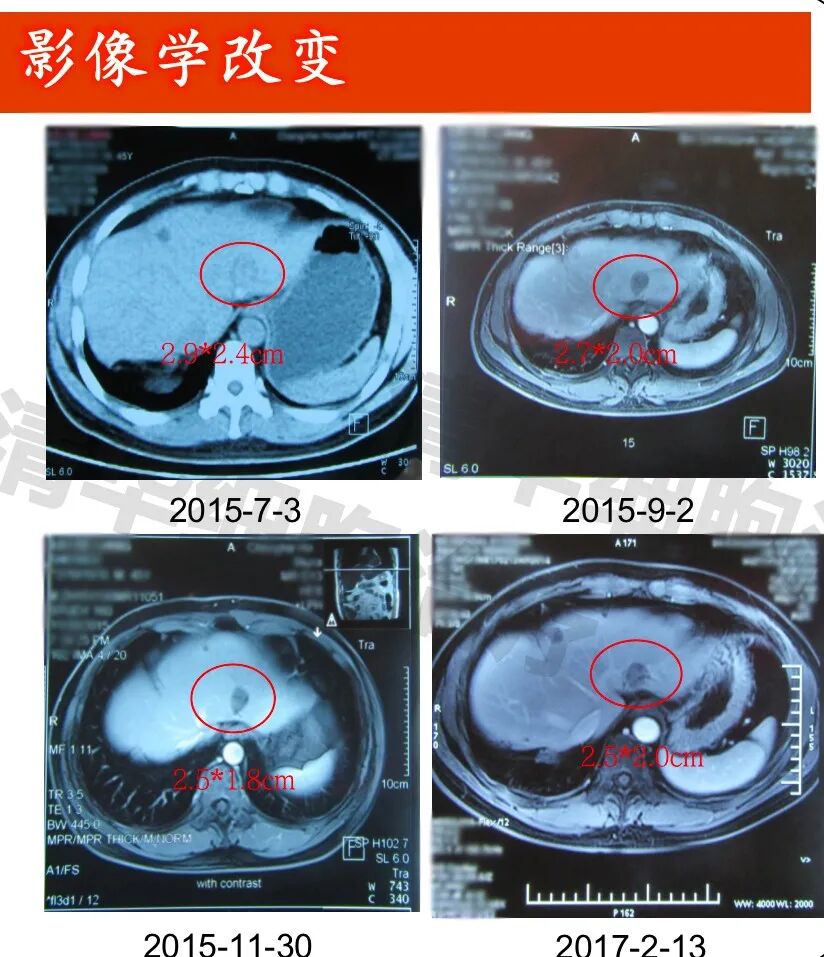
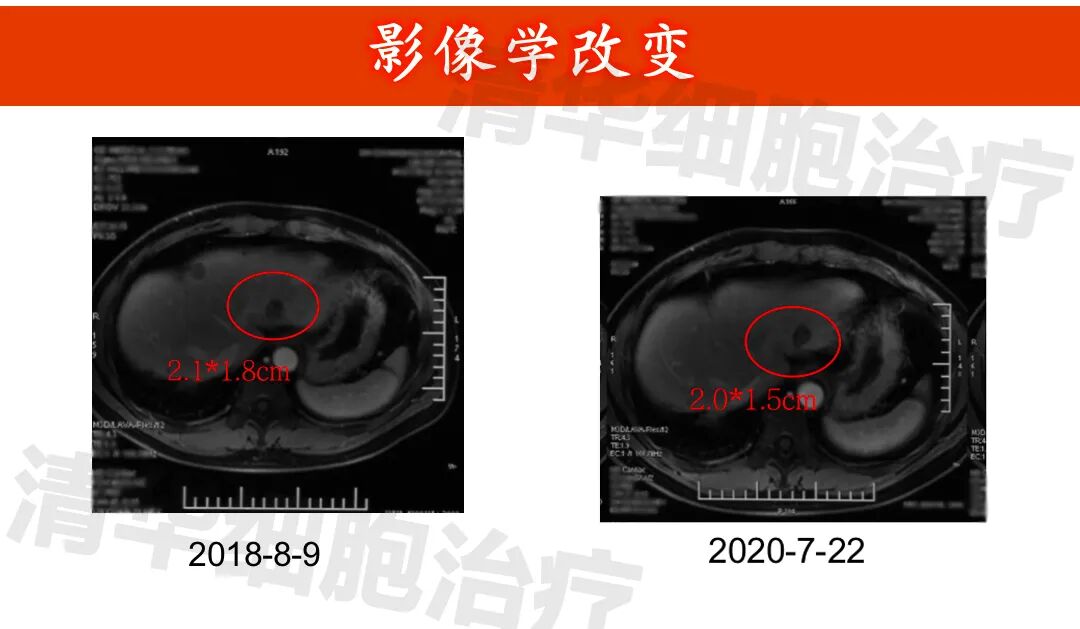
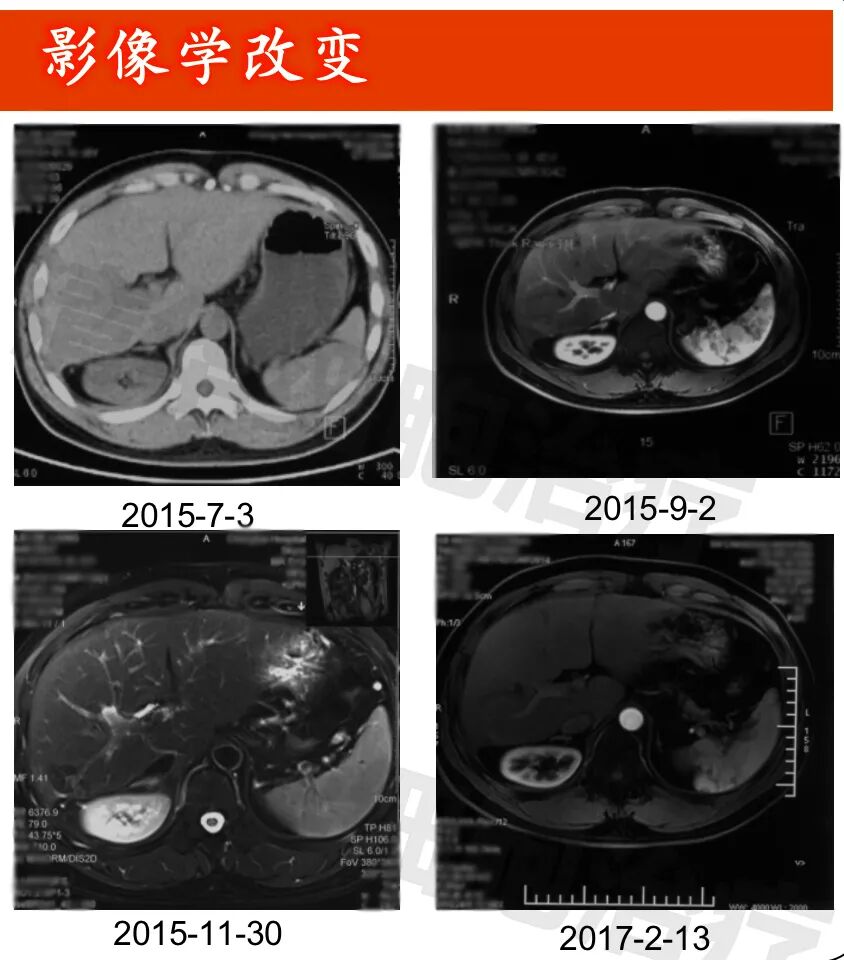
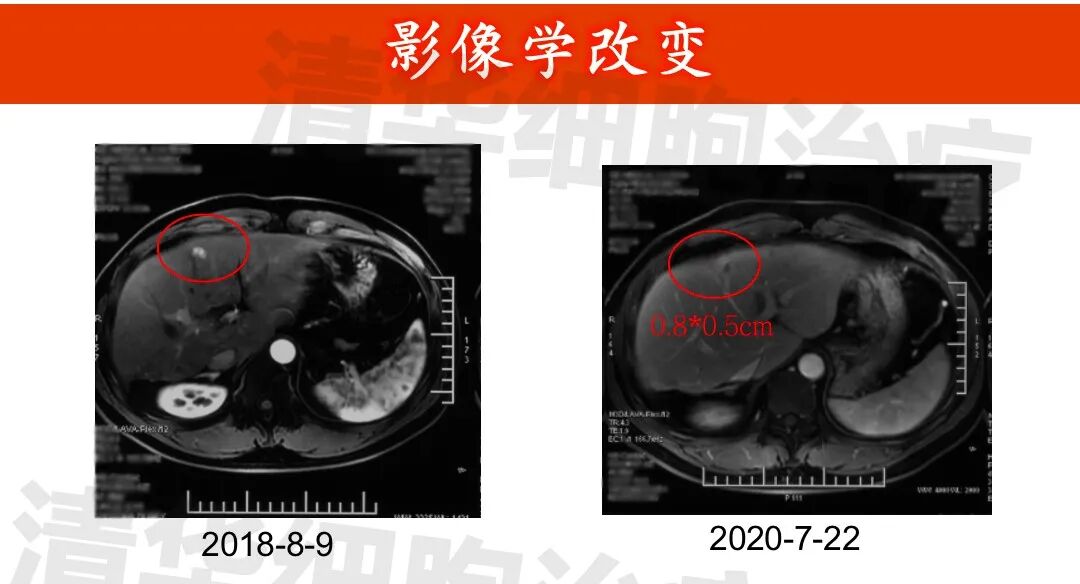
Imaging data
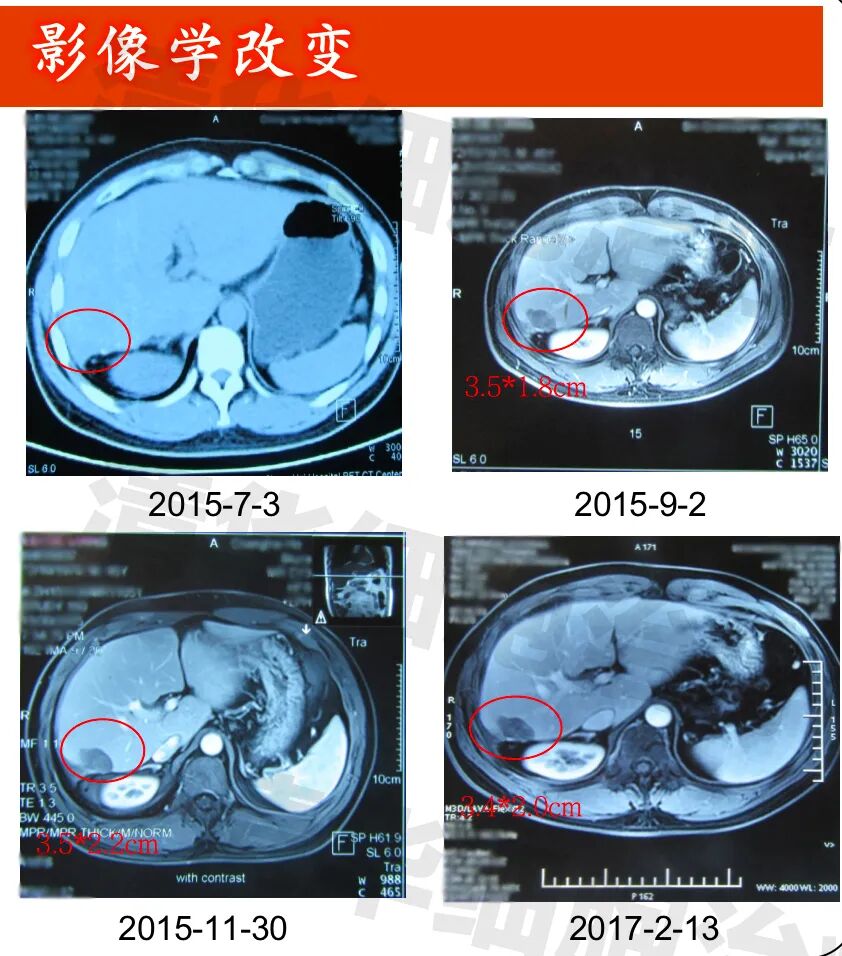
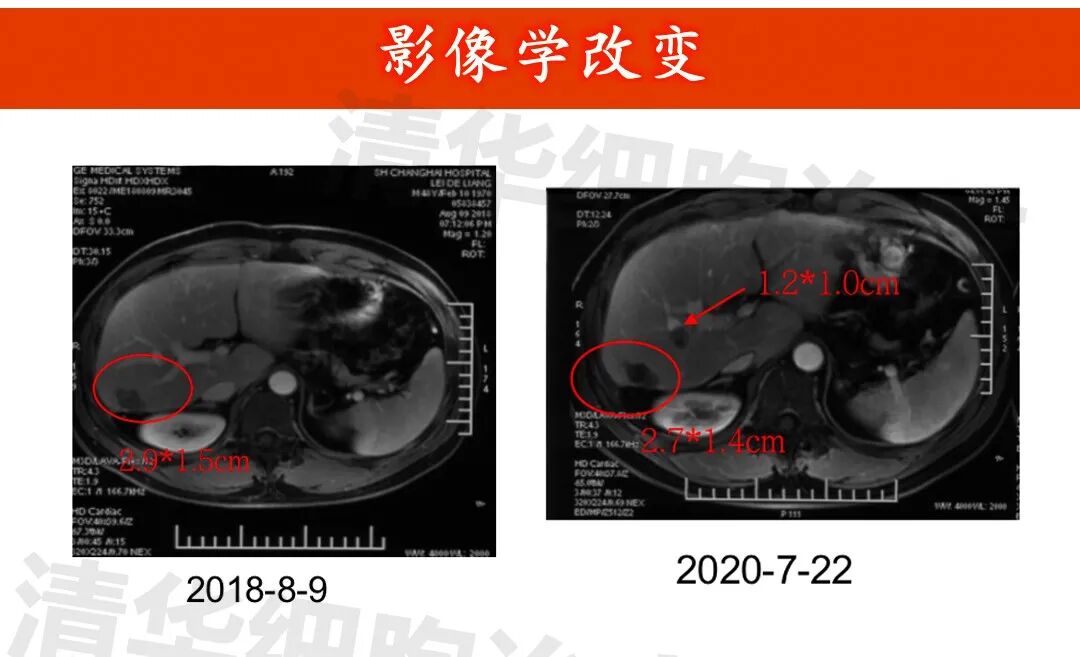
▲Lesion 1 in the right lobe of the liver: 1. On July 3, 2015, a PET-CT scan was performed, but the lesion was not clearly visible and was not measured. All other examinations were MRI scans; 2. The lesion showed post-treatment changes, with no significant abnormal enhancement observed, and the size of the lesion did not change significantly.New lesion in the right lobe of the liver: approximately 1.2*1.0cm in size (indicated by the red arrow), regular monitoring is recommended.

Click on the image
to view

Popular science is a form of charity
<<<Long press to scan QR code
Follow Tsinghua Cell Therapy
