About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。

If you cannot understand the subsequent professional descriptions, you can just spend two minutes to read through this text.
Overview of the condition
knowledge
Breast BI-RADS Grading
Breast BI-RADS Grading is a widely recognized classification system for breast diseases in ultrasound, radiology, and clinical practice. During color Doppler ultrasound (CDUS) examination, breast nodules can be classified into 1-6 categories. Most of the 1-3 category breast nodules are relatively common benign diseases that do not cause serious complications, so patients can undergo regular CDUS follow-up without excessive treatment. Category 5 breast nodules have a high risk of being malignant, and Category 6 nodules are almost certainly breast cancer. Patients are advised to undergo surgical removal of the diseased tissue in a timely manner. Category 4 nodules are generally difficult to determine, but they also have a high risk of being malignant. Typically, BI-RADS Category 4a is an indication for surgical treatment.
1. The patient was diagnosed and underwent surgery in 2019. Postoperative pathology indicated lymph node metastasis and vascular cancer thrombus, which are risk factors for future metastasis.
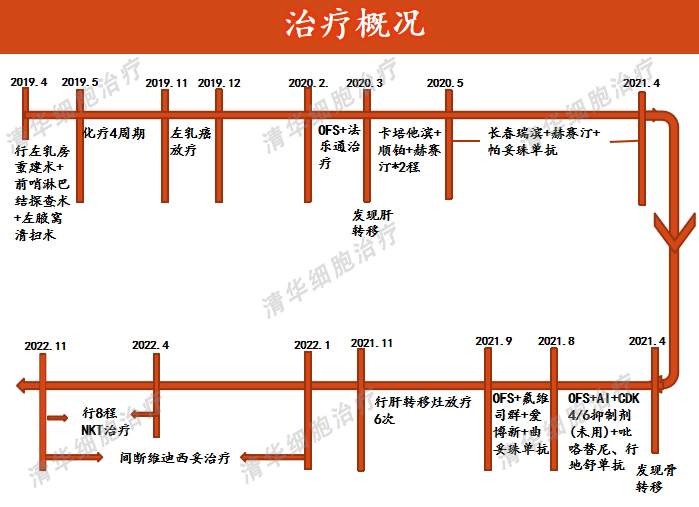
2. The patient has experienced multiple recurrences after surgery and has undergone two surgical treatments, as well as various treatments such as multiple rounds of chemoradiotherapy. Currently, tumor lesions still persist.
3. Recurrence after multiple treatments indicates a high malignant potential of the tumor, making it difficult to control tumor progression with conventional treatment alone.
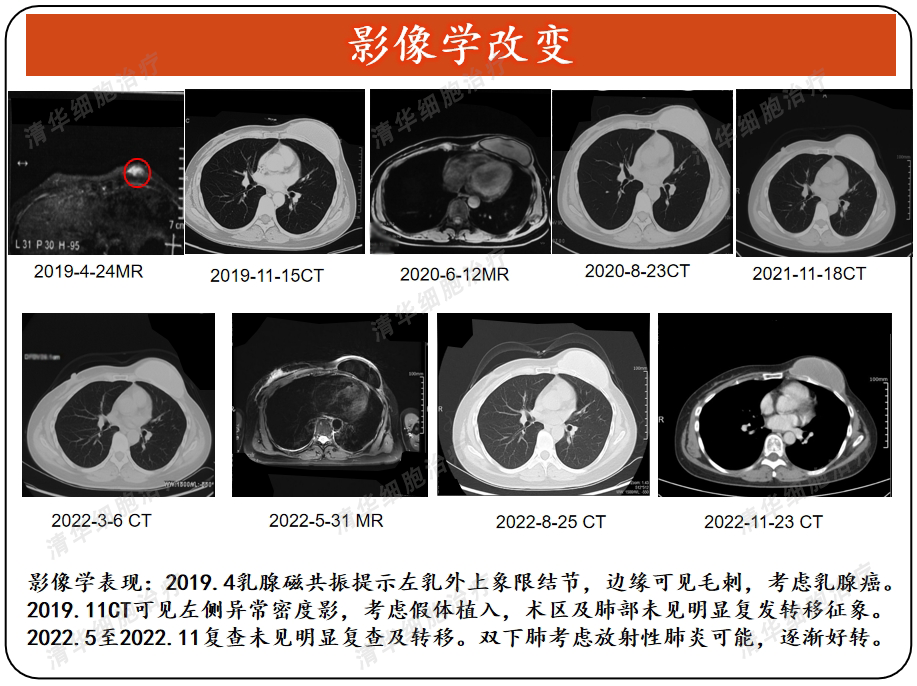
Imaging
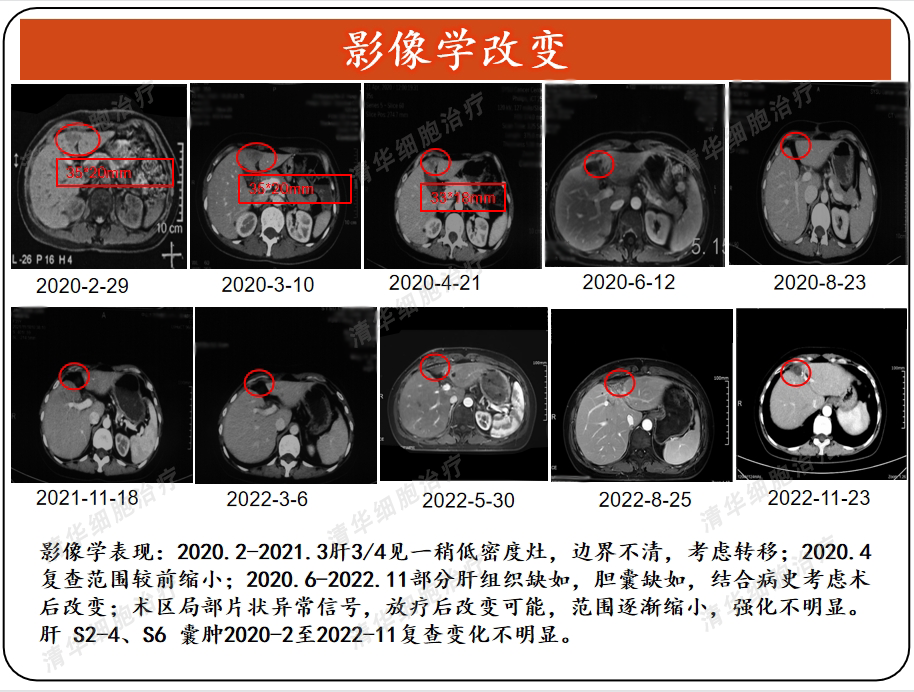
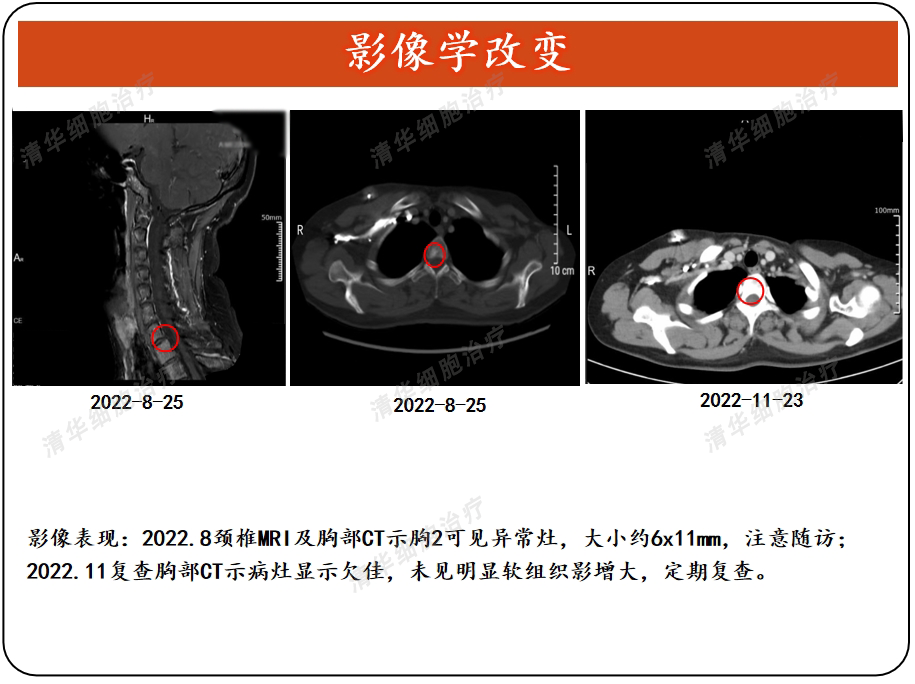
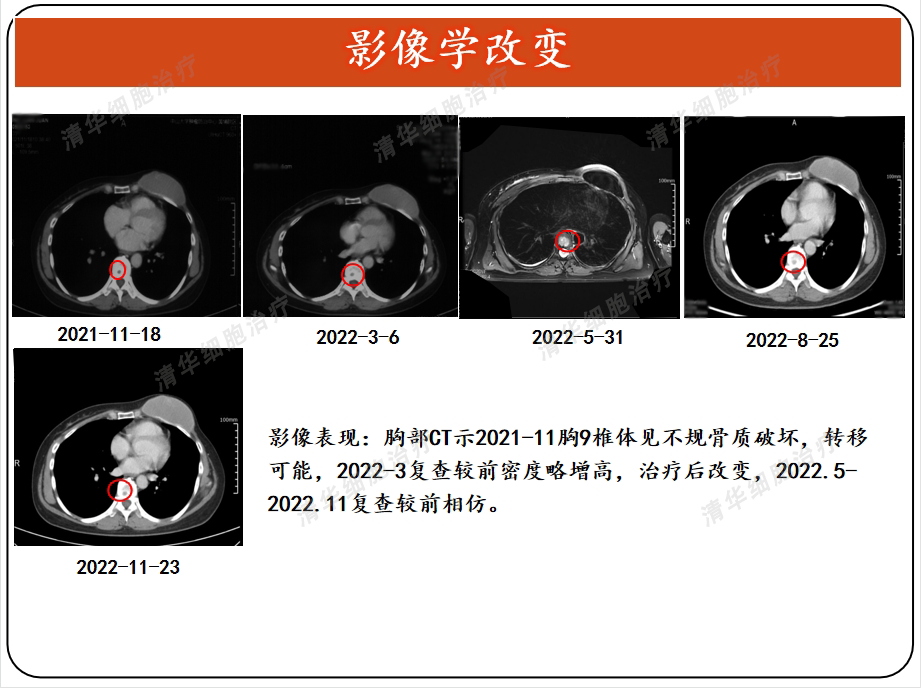
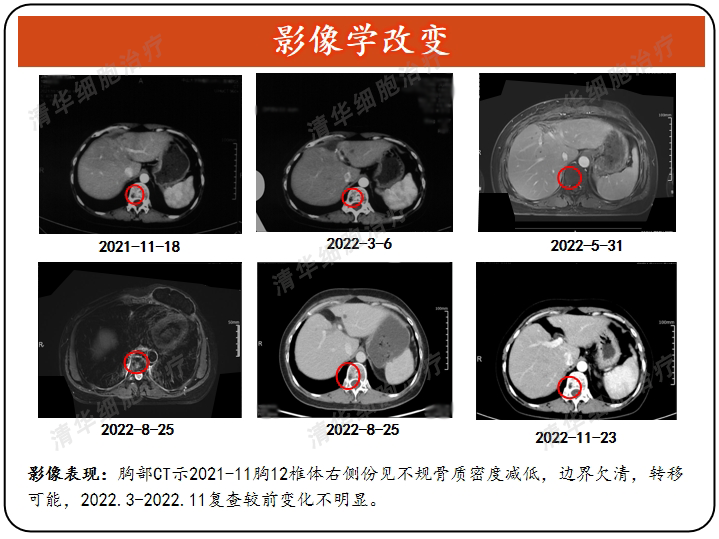
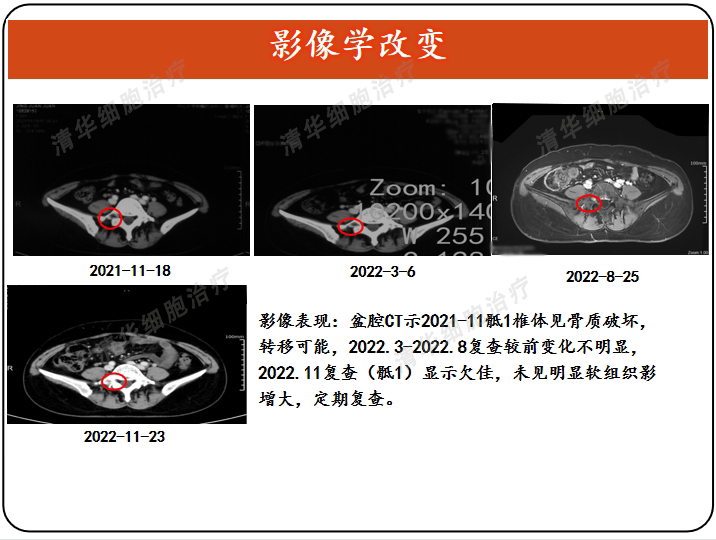

Tumor markers
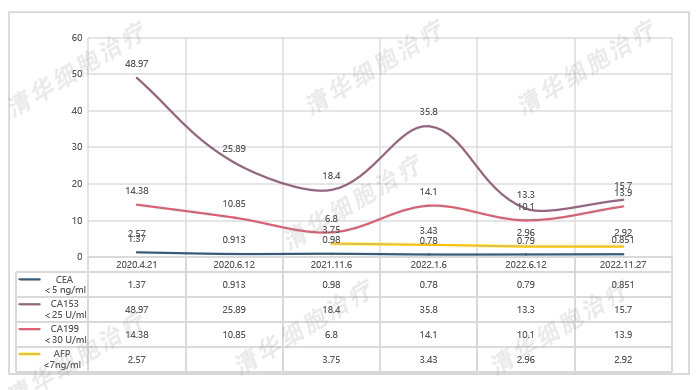
Conclusion and Comments
Reference:< H400>
【1】Qu, Y., Zhao, D., Mu, J., Che, N., Zhang, C., Liu, Z., Su, D., Zhou, L., Zhang, H., & Wei, L. (2016). Prognostic analysis of primary mucin-producing adenocarcinoma of the lung: a comprehensive retrospective study. Tumour biology : the journal of the International Society for Oncodevelopmental Biology and Medicine, 37(1), 887–896.
Click on the image